When palpation isn’t enough: understanding soft tissue changes in children
When human tissue, such as muscles or some organs, are affected by disease, they can become stiffer (or softer) than surrounding muscle tissue. Traditionally, medical practitioners have used the palpation technique – using their hands to determine the firmness of tissue, for instance around the abdomen – to feel for changes in tissue stiffness in order to diagnose illness or disease. Cancers, for example, are often first detected by palpation.
While this is an effective technique, not all tissue is accessible to a physician’s hand. In these cases magnetic resonance elastography (MRE), a non-invasive medical imaging technique, has been developed to assess the stiffness of tissue such as the liver, muscles, or brain.
My team is particularly interested in changes in tissue stiffness in the brain and muscles and how this changes in neurological and muscle disorders. During our research we came to realise that while there is a lot of data on stiffness in adult tissue, there was little to none when it came to children. To answer this we are working on new methods to measure the properties of tissue when it is in use or under stress, either as a result of injury or disease. 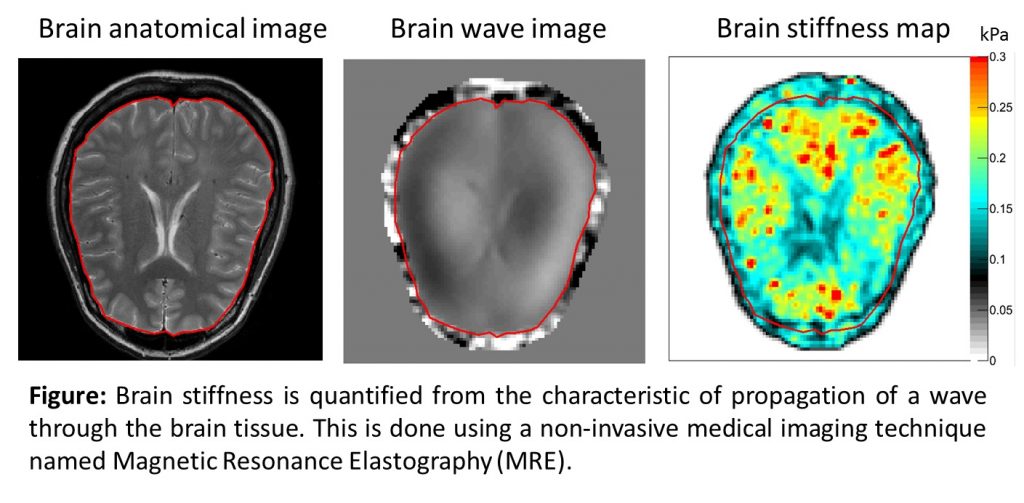
Understanding how the soft tissues of the human body behave mechanically during normal development is a key way to fully understand what happens during growth, injury or the body’s response to disease. It also gives us ‘reference values’ that we can compare a sick child’s scan results to, to help us know whether something is abnormal. We showed recently that this is important for diagnosis of liver disorders in children, since children’s livers do not have the same stiffness as adult livers.
One of the areas we are particularly interested in studying involves keeping children safe during car accidents.
Current injury criteria and anthropomorphic test dummies, for example, are based on scaling adult anatomy to match children’s anatomy. Despite this, the dummies use adult tissue properties, even though there is evidence that this can result in flawed injury criteria that cannot predict injury outcome in real children.
To date, we have completed the skeletal muscle and liver studies, and are currently working on the brain study.
This involves using MRE and diffusion tension imaging (DTI) to find a more accurate way to assess and measure soft tissue changes in children. This involves using an MRI scan of 40 children aged between 5 and 18 years of age. Children younger than five may find it difficult to stay still for the required amount of time. We’ll then compare these scans with ones of adults aged 21 to 50 years of age to see what differences there are in tissue stiffness.
Subjects will be in the MRI scanner for about 45 minutes in total, including 10-15 minutes to set everything up, and a series of scans lasting around 3 minutes per segment with short breaks in between.
In doing this, we will quantify the mechanical properties and microstructure of tissues in healthy children in order to better predict the responses of these tissues in situations such as car accidents or disease, and provide better diagnostic tools for doctors. This information will allow us and other researchers to create accurate computer models of the body for use in child injury prevention, and better differentiate healthy and unhealthy tissue in scans.