5 things you didn’t know about back pain
1. Feeling anxious or depressed about your back pain during your first consultation with your GP? You’re likely to need more visits and medical attention than someone who feels relatively chilled about the whole thing. A study of 2891 patients with back pain revealed that a person who felt very anxious would consult with healthcare practitioners 50% more frequently over three months than someone with similar pain levels and no anxiety about the problem. Similarly, someone who felt very depressed would consult with healthcare practitioners 30% more frequently over three months. This tells us that GPs need to address this emotional distress in the initial consultation, which will reduce costly and potentially unnecessary future healthcare use for patients.
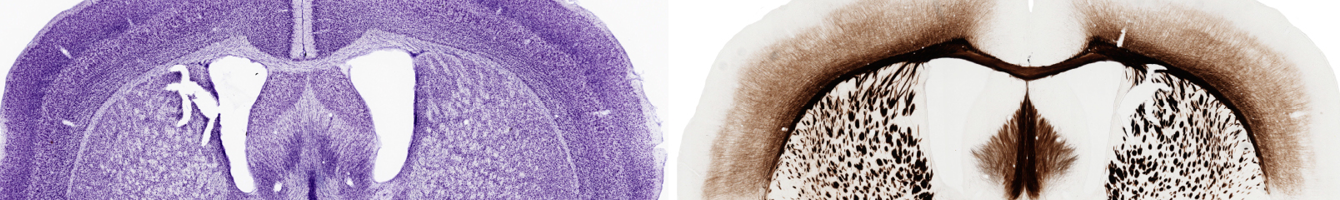
2. Long-term back pain has an effect on your brain. Dr James McAuley was involved in an international study that examined the relationship between chronic back pain and the volume of grey matter in particular areas of the brain. The study found that people with back pain had decreased volume of grey matter in areas of the brain associated with producing pain – for example areas associated with the anticipation and unpleasantness of pain – as well as emotional regulation and with cognitive processing. This tells us that the brains of people who have had back pain for a long time process everyday experiences differently from those who don’t have pain, which could contribute to the development and maintenance of back pain.
3. Having a good GP who spends just 10 minutes explaining how pain works and the part your brain plays in perceiving this pain will make you feel more confident about your outcomes than having a scan or X-ray. NeuRA researcher Adrian Traeger combined the results of 12 randomised control trials, which included over 3,000 patients, and found that a very brief intervention at the doctor’s office for as little as 10 minutes could reassure patients for up to a year. Most of the studies he reviewed used a ‘biopsychosocial’ education model, where the GP explains how physical factors are only one part of the problem – that thoughts and feelings also contribute to the experience of back pain. Traeger and colleagues have developed a patient education model that explains how the brain is involved in pain and are currently testing this in a randomised clinical trial.
4. Preventing back pain could start with a single tweet. In the future we may be able to identify, via their twitter stream, when a person is about to experience a new episode of back pain and send them helpful, timely advice about protecting their back before anything happens. Hopin Lee conducted a study of more than 742,000 Twitter users and identified key words that indicated a person was highly likely to injure their back. Using real-time surveillance methods future e-health providers could tweet educational materials to the at-risk Twitter users to improve their awareness of potential back pain risks and how to avoid them.
5. NeuRA researchers have developed a way to predict whether your back pain is likely to last. The online tool, called PICKUP, uses five questions to estimate the risk of your back pain lasting longer than three months. A version of the online tool is available for both patients and GPs. Along with personalised data about expected recovery, the tool includes information on treatment options to help you plan your recovery. The aim is to allow you to make informed decisions about how much healthcare you need. If you have an above average risk of a slow recovery you can decide, at an early stage, whether you might need more more intensive intervention like physiotherapy. On the other hand, if you have a very good prognosis, you might opt to manage the problem yourself. A preliminary validation of PICKUP was published in PLOS Medicine and estimated a 40 percent reduction in unnecessary medical interventions if GPs used this tool to discuss the expected outcomes with their patient.
Thank you for your insights.
What references do you have for these insights? I am not able to fact check what you are writing because there are no references.
I am quite sure that you are misinterpreting insight number 4 as it is not possible for us to predict injury very well in generel and I would highly doubt tweeting information would inform us when we are at risk of having an injury occuring.
Injury is not the same as pain and pain is not the same as injury. This is of course semantics but it perpetuates biomedical beliefs that pain is only due to injury and that pain comes from the body. I would highly recommend you altering the phrasing of number 4 as it is not up to date with current science and does not provide information that is beneficial or valuable to patients nor health care professionals. Giving advice that focuses on protecting the back can actually increase patient hypervigilance and be a part of why they experience back pain. Instead advice focusing on what positives one can do for one self would be a better option.
This study provides some evidence for the above claim and I can link to more studies if necessary http://www.ncbi.nlm.nih.gov/pubmed/24218376
It is very interesting though a tweet may give us information on increased risk of recurrence of pain and it may be possible we can use this information to decrease the risk of back pain recurrance.
If possible I would very much appreciate the references for the claims provided in this article.
Thank you
Kind regards,
Simon Kirkegaard
Thanks for your comment Simon. Please see the links to the relevant references below. Also, please see a direct response from lead author Hopin Lee to your comment on the twitter paper below.
1. http://www.ncbi.nlm.nih.gov/pubmed/26940056
2. http://www.ncbi.nlm.nih.gov/pubmed/26476265
3. http://www.ncbi.nlm.nih.gov/pubmed/25799308
4. http://www.ncbi.nlm.nih.gov/pubmed/26661720
5. http://www.ncbi.nlm.nih.gov/pubmed/27187782
I think the finer details of our study got lost in communication. You are right about the important distinction between injury and pain. In our study we simply set out to predict “self-reporting back pain”. It is unclear whether these unsolicited self-reports of back pain reflect a true “injury” or a “painful experience”. I suspect we may have captured a combination of the two constructs. It is also important to note that they are not entirely mutually-exclusive constructs. Despite the well documented mantra: “injury does not correlate with pain”.
For more details…
Here is the full paper: http://jamia.oxfordjournals.org/content/early/2015/12/11/jamia.ocv168
And an exclusive blog we posted some time ago: http://www.bodyinmind.org/tweeting-back-pain-study/
Best wishes
Dr Markus Hübscher
Postdoctoral Fellow
Conjoint Lecturer, Prince of Wales Clinical School | UNSW
NeuRA
Good reads! I enjoy reading your post. Which means, before your back pain got severe, self medication is not advisable. As I research on the internet, there are many suggestions or activity like exercise to ease the pain. What kind of Doctor needs to consult for severe back pain? Surgery is the last option? Thank you for the great insights.