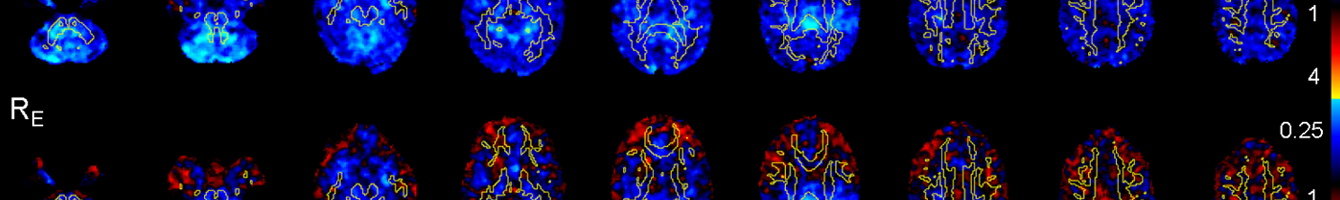
Using DTI to understand muscle contracture in children with Cerebral Palsy
A new study by Prof Rob Herbert and his team is investigating muscle contracture in children with cerebral palsy. Contracture is a stiffening of muscles, even when the muscle is passive. It is not yet known whether contracture is a result of changes in the muscle, changes in the associated tendon, or a combination of both. Around 53 per cent […]
Read more